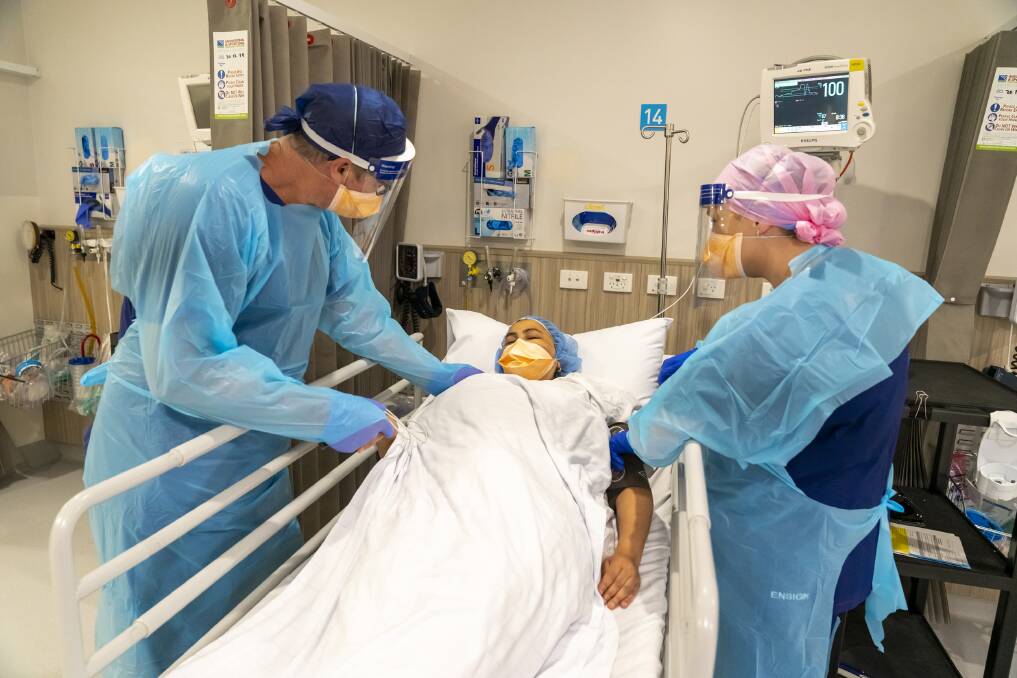
It has been a familiar story across hospitals since COVID-19 forced communities into lockdown.
Non-urgent operations were delayed and the elective procedure backlog was growing.
Yet what also arose was a bubble of confusion, with staff stating that mixed messages that caused internal disputes during the height of the pandemic.
Recent data reveals more people are choosing to fork out funds to access the private health system over public hospital queues.
Figures show Australia's private hospitals have boosted their efforts to address the elective surgery backlog.
The Australian Prudential Regulation Authority revealed there were 995,540 episodes of care in private hospitals during the three months to the end of September. This is an increase on the previous quarter, even though restrictions were in place during the quarter in NSW.
Hurstville Private Hospital, owned by Healthe Care, was among those that deferred procedures, but it also had to alter new ways of working, in what was an unexpected and everchanging period.
Chief executive officer, Lloyd Adams, said the past 18 months was a "traumatic time".
He said while things are much clearer this time around, there was some conflicting information from NSW Health during the first two Sydney lockdowns.
"Hurstville was in the middle of a high risk LGA area," Mr Adams said.
"Restrictions on elective surgery wasn't thought out properly so we had to make our own decisions on what we had to stop.
"I stepped up restrictions in our hospital because we have maternity and ICU, including high risk cardiac patients, so we had to protect our staff and patients."
He said while category 3 procedures such as plastic surgery or dental were deferred, there was ambiguity in the air.
"A category 1 procedure such as giving birth or cardiac surgery was clear. But for example a doctor treating a patient who had prostate cancer, may have considered them to be a category 1, but oncologists would say it's category 2b, so there were conflicting messages," he said.
"Or urologists would classify kidney stones as category 1 but under NSW Health guidelines it was deemed category 2b.
"That's very low. In the private sector acute kidney pain equates to childbirth. You just want to get it done."
He said as a result, some arguments would occur. "Some doctors were dobbing on each other. We felt bad for the community because patients were upset that the surgery they would normally be able to have wasn't able to be done."

With elective surgery getting back on track, Mr Adams said the effects on staff had taken a toll.
"We have all this additional work which is great, but it's terrible for our workforce because they've never really had a break. Everyone is under the pump," he said.
"We made sure during all the challenges we looked after our 450 employees. For example, we provided an open kitchen for staff to take home meals to their families."
With the brakes on migrant intakes, skilled health workers who would normally be placed in the hospital, would mean management had to re-think some existing roles.
"We had a shortage in nurses and midwives because normally what we'd get in from England for example, they weren't coming in, and there was a huge baby boom during lockdown," Mr Adams said.
"So we bolstered up our nursing staff. We trained a lot of our nurses to do basic Mothercraft support alongside our midwives."
He also said the demand for elective procedures was high even before lockdown.
"Regardless of COVID-19 we have been doing public hospital work," he said.
"The backlog has always been there and has fallen into our laps. Now it's just exacerbated. We're happy to help but our priority is our private patients."
To help patients access the private health system, Hurstville Private was the first in Australia to launch Self-Pay Surgery, which gives uninsured patients the opportunity to pay upfront for necessary procedures.
A popular model in the UK, it is a similar to how a private health fund operates, but without having to wait several years for a common procedure.
"Typically the biggest waitlists are for orthopedic, ophthalmology or diagnostic screening," Mr Adams said.
"It's an issue that will be around for two to three years."
A spokeswoman for Ramsay Health Care, which has St George and Kareena private hospitals under its banner, said both hospitals were working with its doctors to ensure they have access to as much theatre time as possible in order to schedule surgeries for their patients as appropriate.
"We have also been assisting NSW Health throughout the COVID-19 pandemic by admitting and operating on public patients in our hospitals to help reduce the backlog of surgeries in the public health sector," she said.

